Genetics and Developmental Pediatrics Research

Would you like to participate in research opportunities available through the Division of Genetics and Developmental Pediatrics? Click the link below to provide us with preliminary information and we will contact you when we have available studies you or your child may qualify for.
Research Highlight
Current Research Projects
ADDM
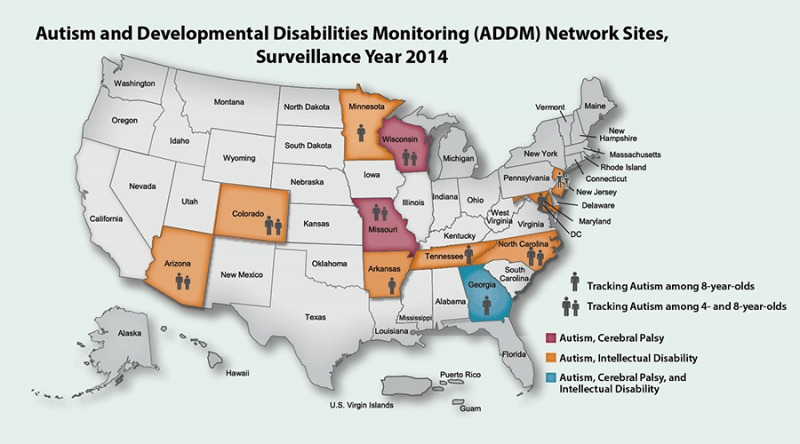
The Autism and Developmental Disabilities Monitoring (ADDM) Network is a group of programs funded by CDC to estimate the number of children with autism spectrum disorder (ASD) and other developmental disabilities living in different areas of the United States. Arizona has been a member of this network for over 20 years, one of the few sites to be involved in every prevalence study year since the project’s inception.
Manuscripts published in the past five years
Upcoming talks and presentations
MD STARnet
The Centers for Disease Control and Prevention (CDC) funds the Muscular Dystrophy Surveillance, Tracking, and Research Network, known as MD STARnet. MD STARnet collects critical information about muscular dystrophy that will improve care for those living with the disease. Arizona served as an abstraction site between 2002 and 2014 and currently collaborates on analyses with the New York MD STARnet site run by the New York State Department of Health in Albany.
Manuscripts published in the past five years
IHD
The division is collaborating with the Institute for Human Development at Northern Arizona University on research performed under the Arizona University Centers for Excellence in Developmental Disabilities Education, Research, and Service (AzUCEDD). We have collaborated as the clinical arm of the IHD since 1990 and look forward to our continued relationship. The video below highlights projects and division staff activities.
MCH Got Transitions
In the 2017 Title V Block Grant Applications, the Arizona Department of Health Services, Bureau of Women and Children’s Health selected transition as a targeted performance measure for youth with special health care needs. The purpose of this project is threefold: 1) to evaluate the current proportion of practitioners in Arizona who have a formal transition policy; 2) to determine the impact of existing transition polices; and 3) to develop and pilot a transition implementation program to assist practitioners without policies to incorporate transition into regular practice. The project utilizes the Got Transition tools. Got Transition/Center for Health Care Transition Improvement is a cooperative agreement between the Maternal and Child Health Bureau and The National Alliance to Advance Adolescent Health.
Curemark
We served as a Phase III clinical trial site for Curemark’s CM-AT. Curemark’s lead drug candidate, CM-AT, has received “Fast Track” designation from the U.S. Food and Drug Administration (FDA). FDA has also granted Curemark a rolling review of its New Drug Application for CM-AT. Please click on the link above to learn more about how CM-AT treats some of the core symptoms of Autism.
 Contributions
Contributions
2013 Predictors of Ascertainment of Autism Spectrum Disorders Across Nine US Communities. Link
2014 Prevalence of autism spectrum disorder among children aged 8 years - autism and developmental disabilities monitoring network, 11 sites, United States, 2010. Link
2015 The validity and usefulness of public health surveillance of autism spectrum disorder. Link
2015 Autism spectrum disorder prevalence and proximity to industrial facilities releasing arsenic, lead or mercury. Link
2016 Prevalence and characteristics of autism spectrum disorder among 4-year-old children in the autism and developmental disabilities monitoring network. Link
2016 Prevalence and Characteristics of Autism Spectrum Disorder Among Children Aged 8 Years—Autism and Developmental Disabilities Monitoring Network, 11 Sites, United States, 2012. Link
2016 Autism Spectrum Disorder prevalence and associations with air concentrations of lead, mercury, and arsenic. Link
2017 Autism spectrum disorder reporting in lower socioeconomic neighborhoods. Link
2017 DSM criteria that best differentiate intellectual disability from autism spectrum disorder. Link
2018 Prevalence of autism spectrum disorder among children aged 8 years—Autism and Developmental Disabilities Monitoring Network, 11 Sites, United States, 2014. Link
2018 Characterizing Health Disparities in the Age of Autism Diagnosis in a Study of 8-Year-Old Children. Link
2018 Automated Extraction of Diagnostic Criteria From Electronic Health Records for Autism Spectrum Disorders: Development, Evaluation, and Application. Link
2013 Oral corticosteroids and onset of cardiomyopathy in Duchenne muscular dystrophy. Link
2013 Patterns of growth in ambulatory males with Duchenne muscular dystrophy. Link
2014 Correlates of care for young men with Duchenne and Becker muscular dystrophy. Link
2014 Sibling concordance for clinical features of Duchenne and Becker muscular dystrophies. Link
2014 Complementary and alternative medicine for Duchenne and Becker muscular dystrophies: characteristics of users and caregivers. Link
2014 Diagnostic and clinical characteristics of early-manifesting females with Duchenne or Becker muscular dystrophy. Link
2015 Prevalence of Duchenne and Becker Muscular Dystrophies in the United States. Link
2016 Health services received by individuals with Duchenne/Becker muscular dystrophy. Link
2016 Rehabilitative technology use among individuals with Duchenne/Becker muscular dystrophy. Link
2016 Respiratory Care Received by Individuals with Duchenne Muscular Dystrophy (DMD) from 2000 – 2011. Link
2017 Perceived quality of life among caregivers of children with a childhood-onset dystrophinopathy: A double ABCX model of 7 stressors and perceived resources. Link
2018 Duchenne and Becker muscular dystrophy in adolescents: current perspectives. Link
2018 Implementation of Duchenne muscular dystrophy Care Guidelines at selected sites in the United States. Link
2018 Diagnostic Accuracy of Phenotype Classification in Duchenne and Becker muscular dystrophy using medical record data. Link
2018 A Review of MD STARnet’s Research Contributions to Pediatric-Onset Dystrophinopathy in the United States; 2002-2017. Link